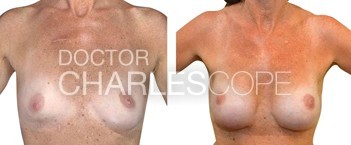
Recent changes in reconstruction surgery
Breast reconstruction has changed in the last ten years, with the reconstruction rate of patients with early breast cancers increasing significantly, reaching 30-50% of patients in some units.
As well as the increase in reconstruction there have been three other changes:

- Skin-sparing mastectomy and nipple-sparing mastectomy are being performed with earlier cancers/DCIS. These type of mastectomies remove less skin or no skin with the breast tissue, and Dr Cope recommends combining these with immediate reconstruction to give the best possible cosmetic result*. It may also reduce the need for surgery on the other breast to achieve a symmetrical result*. There have been two large studies which have shown that skin-sparing mastectomy does not affect the treatment of early breast cancer. This technique, however, is only suitable for patients with very early breast cancer.
- Immediate reconstruction (at the time of mastectomy) is being used more because it often has better results*. Immediate reconstruction may decrease the number of operations involved, though it may increase recovery time. Again immediate reconstruction has been shown not to affect treatment of early breast cancer. Immediate reconstruction can also decrease some of the psychological impact of mastectomy, and allows a quicker emotional adjustment to the diagnosis of breast cancer and return to normal life*. It means patients can avoid wearing external prostheses, and wear normal clothes and resume normal activities, such as swimming.
- Prophylactic (preventative) mastectomy on the other (normal) breast is being performed increasingly to reduce the risk of having another breast cancer in the other breast, with the added advantage that it provides a better symmetry and cosmetic result of the reconstruction*.
There have been a number of studies looking at the benefits of breast reconstruction, which have shown that these patients have significant increases in emotional well-being, vitality, general mental health, functional well-being, and body image compared to those patients without reconstruction(1).
*Note results vary from patient to patient
Decisions in reconstruction
This depends on the individual patient’s situation, however, these days many mastectomies are performed for very early cancers or precancerous changes, and if a “skin-sparing mastectomy” with immediate flap reconstruction (see below) is performed, the patient wakes up after the operation with a breast that looks as similar as possible to before their operation*.
It used to be said that a women should live without a breast for at least a year or more before a reconstruction was done, because of worries of reconstruction delaying detection of local cancer recurrence. There are now studies in large numbers of patients with early breast cancer showing no increase in local recurrence with skin-sparing mastectomy and immediate reconstruction. In general, Dr Cope advises patients to have immediate reconstructions, as they have better results compared to delayed reconstructions*.
Delayed breast reconstruction can be performed any time after mastectomy, and reconstruction should be delayed it is known that radiotherapy will be given after the mastectomy, or if the patient needs more time to make a decision about the options.
There are three main choices, which all have advantages and disadvantages, and most types of breast reconstruction take at least 2 operations to complete.
These decisions are made on an individual basis, depending on many factors, including the position and particular type of cancer, the patient’s general medical health, the size and shape of the patient’s breasts, and the patient’s lifestyle and wishes. Dr Cope will work through these options will you, to tailor the best solution for your individual needs.
*Note results vary from patient to patient